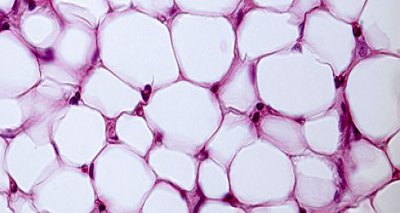
Mechanisms and functional relevance of immune metabolism
It is well established that the presence of obesity greatly increases the risk of insulin resistance and type 2 diabetes. An important contributing factor to the development of insulin resistance is a chronically elevated state of inflammation originating from the expanding adipose tissue.
In recent years, our understanding of the mechanisms underlying the development of obesity-induced inflammation has rapidly progressed. In particular, macrophages have received much interest as key players in obesity via their tendency to aggregate around dead adipocytes in so-called crown-like structures. The inflammatory signals released by the infiltrating macrophages and other immune cells are believed to contribute to the development of systemic insulin resistance.
The work in our group within the Division of Human Nutrition and Health is aimed at trying to better define the specific triggers that underlie the development of adipose tissue inflammation and to understand what drives the pro-inflammatory properties of macrophages in obese adipose tissue. More specifically, our research is geared towards characterizing the intracellular changes that occur in macrophages in obese adipose tissue and that may promote the pro-inflammatory trait.
Understanding macrophage function through metabolism
Advances in the field of immunology research have revealed that the phenotype of a macrophage is largely dependent on intracellular energy metabolism and varies from a pro-inflammatory phenotype characterized by cytokine secretion to a more anti-inflammatory phenotype linked to tissue remodeling. Recent evidence has demonstrated that intracellular metabolism of macrophages is a key determinant of their inflammatory traits. Upon stimulation, cellular metabolism of an immune cell undergoes profound changes. These metabolic adaptations are aimed at optimizing immune cell function, including proper bactericidal activity and enhanced cytokine production.
Our current emphasis is on the identification of the intracellular changes that occur in macrophages in lean and obese adipose tissue that may dictate the pro- or anti-inflammatory properties of the cell.
Cleaning up of adipose tissue through phagocytosis
One of the key functions performed by a macrophage is phagocytosis. Phagocytosis is mostly aimed towards foreign pathogens but can also target endogenous cells that are damaged or old and need to be replaced. The clean-up of damaged and old cells is termed efferocytosis and occurs in virtually every tissue in an immunologically silent manner by macrophages attracted by so-called ‘recognize-me’ and ‘eat-me’ signals. Ineffective removal of cells generally promotes the development of inflammation as cells may turn necrotic and attract pro-inflammatory macrophages and various other immune cells. Interestingly, adipose tissue of obese subjects is characterized by an increased number of pro-inflammatory macrophages as well as dead adipocytes, suggesting inadequate clearance. Current research efforts are focused on the identification of the phagocytic machinery in adipose tissue and to unravel to what extent this process is affected during the development of obesity.