
Hepatitis E
Hepatitis E is a liver disease caused by the hepatitis E virus (HEV). HEV occurs sporadically in developed countries, primarily in the genotypes 3 and 4, which originate in animals. Infection with HEV often progresses in general without symptoms. The infection can also lead to an acute liver infection that often causes more serious complications, especially in immunocompromised people.
How many people are affected by hepatitis E?
According to the WHO, 20 million HEV infections, more than 3 million acute cases, and approximately 70,000 deaths are linked annually to hepatitis E. These figures are mainly determined by outbreaks in developing countries. Hepatitis E is transmitted in these countries primarily via drinking water contaminated with excreta. In these countries, the genotypes 1 or 2 of the virus are involved, and these variants occur only in humans.
How do Europeans become infected with hepatitis E?
In industrialised countries, the disease is less prevalent in humans. HEV genotype 3 is the most prevalent type in Europe. Infections may result from eating infected meat or drinking contaminated water. In Europe large differences are observed in the prevalence of HEV, around 5% in Scotland to more than 50% in south east France. In the latter region people are most likely more exposed to the virus through eating raw pork products. Tracing the cause of the infection is often difficult, as the incubation period can take up to 60 days sometimes even longer. The virus can also be transmitted via blood transfusion and organ transplants. Hepatitis E virus genotype 3 has been found, apart from in humans, in domestic pigs, wild boar, certain deer species and shellfish.
How often does hepatitis E occur in the Netherlands?
The number of cases resulting from HEV in the Netherlands is estimated at 1 to 5 infections per 100,000 people per year. Pigs are almost certainly the most important source of these infections. On the basis of various studies, it has been found that HEV occurs on more than 50% of the pig fattening farms in the Netherlands. It seems that targeted intervention measures will be needed to reduce this percentage. Genetic material (RNA) of the virus has been shown in pig liver sold in butchers.
Is treatment available?
The hepatitis E virus can cause liver inflammation in pigs, although evident symptoms are in fact never found in pigs. For this reason, pigs are in fact never treated for hepatitis E. There is also no vaccine available for preventive treatment. Humans that develop serious hepatitis following infection with HEV can be treated with antiviral medication. In Western Europe this result in recovery in most cases. However, this may need long term treatment that can be executed in hospitals only. Uitklappers
Hepatitis E infection
Four types of the hepatitis E virus occur in humans, all within the species Orthohepevirus. Genotype 1 and genotype 2 occur in humans only, exclusively in the tropical regions of Africa and Asia. Genotype 3 and genotype 4 occur in both humans and animals and can be transmitted from animals to humans (zoonotic). In Europe we see genotype 3 viruses virtually exclusively. This type occurs in the Netherlands in domestic pigs and in wild fauna, primarily wild boar and deer.
Within the species Orthohepevirus, three more genotypes 5, 6 and 7 exist, that occur in animals only and not in humans.
Clinical signs hepatitis E
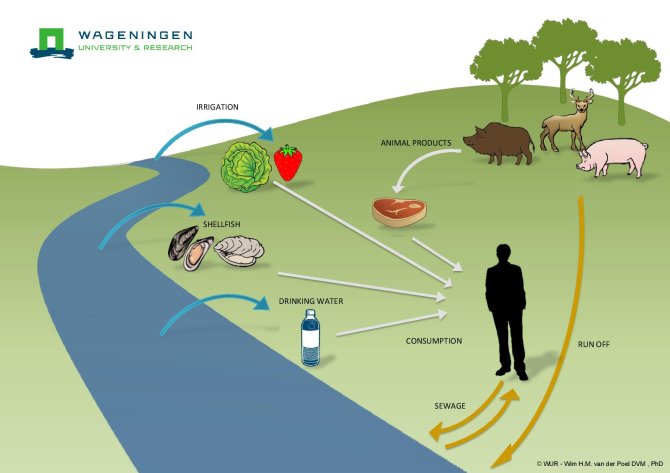
Spread of Hepatitis E
Diagnostics hepatitis E
The hepatitis E virus (HEV) is very difficult to culture. The PCR test is almost always used to show the presence of HEV. The virus (RNA) can readily be shown with the aid of PCR in blood and (liver) tissue samples. Standard procedures have also been developed for the detection of the hepatitis E virus in food and water samples.
For determining antibodies against the hepatitis E virus, various immunoassays, especially ELISAs, are used. Over recent years, these tests have improved substantially, but there are still considerable differences in quality. for the 4 genotypes of HEV occurring in humans, we can only one distinguish a single serotype. Which means that the antibody tests are unable to distinguish between antibodies generated against one of these 4 genotypes. Both the PCR and the antibody tests can be routinely conducted by Wageningen Bioveterinary Research in all the above mentioned samples.
Vaccine hepatitis E
Prevention and control of hepatitis E
Research by Wageningen Bioveterinary Research
Wageningen Bioveterinary Research is conducting research into the transmission routes.The liver is the most important target organ for the virus, although high concentrations can also occur in other organs and in the blood. This means that blood transfusion and organ transplants are also possible transmission routes in humans. Proper heating of infected material kills the virus. Contaminated food eaten raw, for example oysters, forms a potential infection route.
Research into the hepatitis E virus is important in order to find out whether incidence, and so the risk to humans, is rising. In addition, it is important to find out whether virulent variants arise and to gain a better understanding of the (most important) transmission routes.