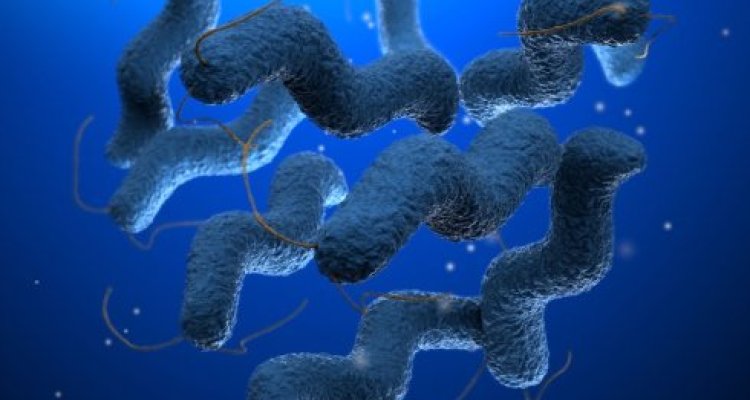
Campylobacter
Campylobacter is an intestinal bacterium which can cause an intestinal infection through contaminated food. The Campylobacter bacteria are the main cause of diarrhoea in humans in the EU and the Netherlands. Most infections come from meat, especially poultry. The government, industry and research work together at national and European levels to tackle infections.
The Campylobacter-bacterium
The Campylobacter lives in the intestines of animals and generally occurs through faeces. The bacterium is also common in foods, but does not develop there.
There are 15 species of Campylobacter, of which Campylobacter jejuni is the most common and is mainly present in birds. This makes chickens the main source of infection.
The disease in humans
Campylobacter can cause campylobacteriosis, an infection of the intestines. Not everyone is equally susceptible to the infection. The disease usually occurs 48 hours to one week after infection. The symptoms range from mild gastrointestinal symptoms to flu, diarrhoea – sometimes accompanied by blood, and abdominal pain. These symptoms can last for five to seven days, and sometimes intestinal cramps will last for weeks.
In exceptional cases, infection with the bacterium leads to the Guillain–Barré syndrome, a deterioration of the nervous system. People with reduced immunity, pregnant women, young children and the elderly are prone to infection with Campylobacter. Every year there are an estimated 25 deaths due to campylobacter infection.
Prevention
The bacterium lives in the intestines of animals and is present in faeces. Upon contact with animals it is therefore important to wash one's hands properly.
Campylobacter is found in raw meat and unpasteurised milk and dairy products. Chicken is the main source of infection. The bacteria can also end up on vegetables through contaminated water. Again, wash thoroughly, avoid raw meat and pasteurise milk. The bacteria die during cooking, baking or roasting. Freezing does suppress the bacteria, but they survive it.
Cross-contamination occurs when knives or cutting boards are first used for the preparation of contaminated meat and subsequently for uncontaminated products, such as vegetables. This is a major source of infection, so use clean utensils for each product.
The risk of infection is greater in Asia and Mediterranean countries; one in six cases of illness is caused abroad.
Advice
- Wash your hands before cooking
- Wash utensils immediately after use with hot water and detergent
- Do not use the same cutlery with raw meat and then prepared food
- Handle the fluids from thawed chicken carefully
- Never use the same surface for raw meat and then cooked food or raw vegetables
- Cook meat thoroughly; do not buy raw milk and raw dairy products, such as butter and soft cheese
- Wash raw fruits and vegetables thoroughly under running water
- Drink tap water abroad only if it is declared safe
- Wash your hands after touching domestic and non-domestic animals, especially if they have diarrhoea