
Longread
Global One Health
Is a course of antibiotics still an effective cure for when I get sick? Are diseases such as avian flu occurring more frequently in the Netherlands? Do mosquito nets really help against the spread of malaria? Can I develop type 2 diabetes?
[2016, reading time: 7 min]
These may appear to be unrelated questions, yet they have much more in common than you might consider at first glance. The underlying health issues for each of these questions cannot be solved with a single approach and neither is knowledge of only veterinary or human medicine sufficient to address these. It is vital that people who specialise in animal health, nature, psychology and plants work together. This is especially important in the field of antibiotic resistance.
Antibiotic resistance
We are seeing it on the news more frequently: the extensive use of antibiotics in livestock farming, GPs raising the alarm regarding the increasing number of patients with multiresistant bacteria and the resistant bacteria in and on our food. What exactly is antibiotic resistance and how do we tackle this issue?
All humans and animals have bacteria. Many of these bacteria are harmless, but some can cause illness and disease. If needed, a GP will prescribe a course of antibiotics to treat a disease or illness. Antibiotics are medication that kill bacteria or stunt their growth, so that people and animals can get well again. One of the most significant disadvantages of this is that bacteria can become resistant to antibiotics. These bacteria are then called resistant bacteria. We now understand that the more antibiotics are used, the greater the chance that bacteria become resistant. This means that an antibiotics treatment is no longer effective and that diseases are becoming more difficult to treat.
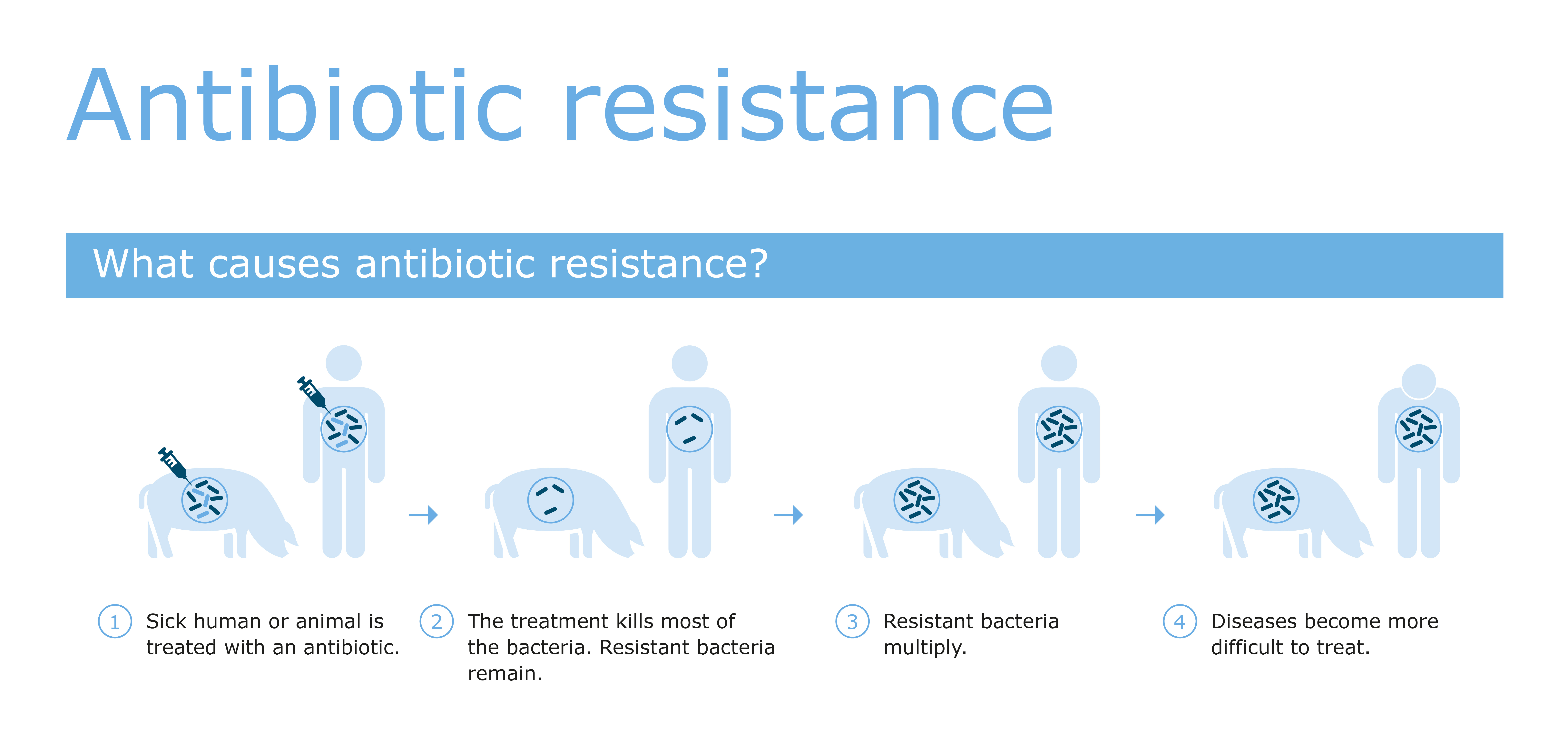
Antibiotic resistance is not a simple problem for which there is a simple solution. It is a complex conundrum that involves livestock farming, healthcare and consumer use but is also further complicated by the fact that bacteria are not hampered by borders in our globalised world. A Global One Health approach is needed to tackle this issue.
What is Global One Health?
Global One Health is a joint initiative of several disciplines to bring about human, animal and plant health in sustainable ecosystems across the world using a chain approach. This approach includes a focus on national and international policies, research and applications.
Institutes for human and animal health are now working together on antibiotic resistance. They are attempting to reduce the use of antibiotics in livestock farming and in the medical field. Through different measures, the use of antibiotics in livestock farming was reduced by 58.4% between 2009 and 2015. In the next few years the focus will be on reducing this number even further. Furthermore, essential human antibiotics may not be used, or are rarely used, in animals.
The use of antibiotics and antibiotic resistance are monitored in both healthcare and livestock farming and jointly reported on in a Nethmap/MARAN report. This allows resistance trends to be monitored and treatments to be adjusted.
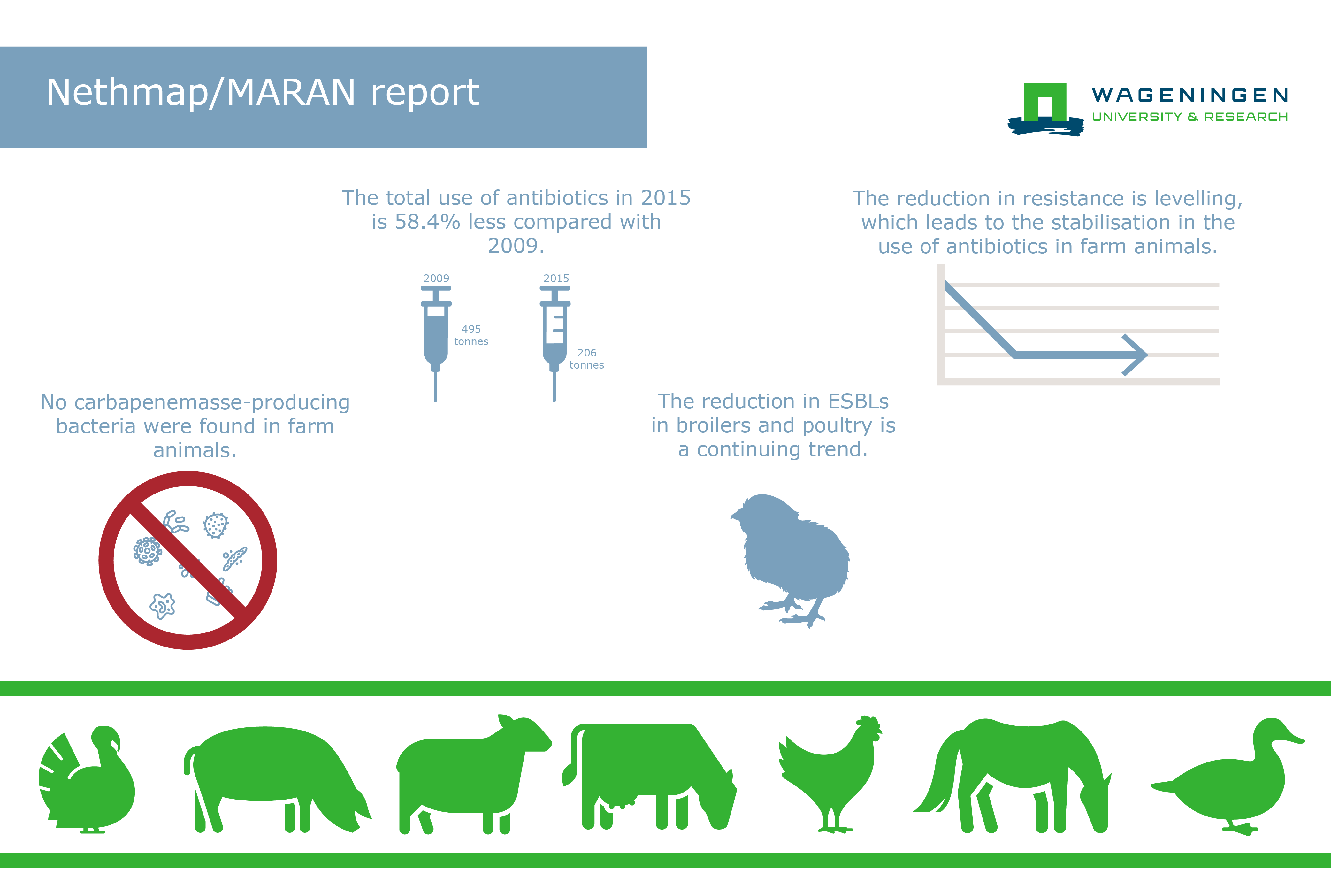
Luckily, there are few cases of resistant bacteria in humans in the Netherlands. This can be attributed to healthcare institutions and livestock farming being informed and alert while closely working together to address this problem. Cooperation helps to reduce the use of antibiotics and to identify trends which means that treatments can be adjusted if necessary.
Read more about antibiotic resistance
Avian flu
A new case of avian flu is a regular feature on the news. Avian flu continues to be a threat to the poultry sector and in some cases presents a health-risk to humans as well. In the Netherlands incidents are usually mild avian flu viruses.
Zoonoses
Diseases that can be transmitted from animals to humans are called zoonoses. Avian flu is an example of such a disease. Other examples include Ebola, tularaemia and Lyme disease. Ebola originated in apes, humans can be infected with tularaemia through hares and rabbits and Lyme disease is transmitted from wildlife to humans through ticks. But animals do not necessarily become ill from zoonoses that harm humans. The hepatitis E virus is an example of this.
There are many different varieties of avian flu. In cases of the H5 or H7 virus, all livestock on a poultry farm will be destroyed, even if it is a mild form. These staunch destruction methods might appear harsh but they are implemented based on European legislation, as a mild H5 or H7 subtype avian flu virus can evolve into a harmful variant. Furthermore, a transportation ban is implemented for a zone of one kilometre or more around the infected farm for the transportation of poultry, eggs, poultry manure and used litter. This prevents the spread and potential outbreak of the flu and contains it quickly and effectively.

Preventing or eradicating avian flu is incredibly complicated. Wild waterfowl act as a reservoir for avian flu viruses. These birds might present nasal discharge at worst but they are capable of infecting poultry. This is especially a high risk for free-range farms. But farms that are not free-range also run the risk of contamination.
A Global One Health strategy with a multidisciplinary and integrated approach is needed in order to better understand avian flu viruses and to restrict their spread and the effects thereof. At Wageningen University & Research vets are working together with ecologists to make the environments of poultry farms unattractive to waterfowl.
Malaria
Estimates by the WHO have shown that there are 198 million cases of malaria around the world each year, resulting in 584,000 deaths. The prevention of malaria is an important but highly complicated matter. The mosquito is the main cause for this conundrum, as it is not easy to combat. The use of malaria medication and insecticides such as insecticide-treated mosquito nets and insect spray have yielded results in the control of malaria. However, high exposure to insecticides has created resistance in mosquitos to these substances. Thus it has become necessary to search for alternative methods for mosquito control.
Once somebody has been bitten by a mosquito, several other factors play a role. If the person is malnourished or has an iron deficiency, the chance of the disease worsening becomes more likely. The health and nutrition of people is an important factor in malaria cases.
Thus, there is no simple solution for malaria. A joint, cross-border Global One Health approach is vital. While research into curative and preventative treatment for malaria is needed, alternative methods for mosquito control, good water management and food production are also important factors. Furthermore, the relationship between malaria, iron and malnutrition needs to be further researched.
Solarmal
On Rusinga Island in Kenya the use of a mosquito trap scented with human body odour has reduced the population of the predominant Anopheles mosquito by 70% in the space of eighteen months.
- Unfortunately, your cookie settings do not allow videos to be displayed. - check your settings
Type 2 diabetes
In addition to infectious diseases such as avian flu and malaria, there are many types of diseases that are not transmitted between people or between animals and humans. These diseases are called non-communicable diseases (NCDs). Cardiovascular diseases, cancer and diabetes are examples of NCDs. These diseases are also a significant risk to human health.
In the case of type 2 diabetes, the body is not able to regulate its blood sugar levels and does not respond adequately to insulin. Insulin is the hormone that regulates blood sugar levels. Diabetes can result in blindness, kidney failure, heart attacks and amputation. The number of people who have type 2 diabetes is growing. In 2014, 422 million people had some type of diabetes (WHO, 2016).
The chance of developing type 2 diabetes is increased by inactivity, poor nutrition, obesity and smoking and the disease is a typical disease of affluence. Compared to the past, work is increasingly sedentary, transportation is evolving and people are eating more unhealthy food.
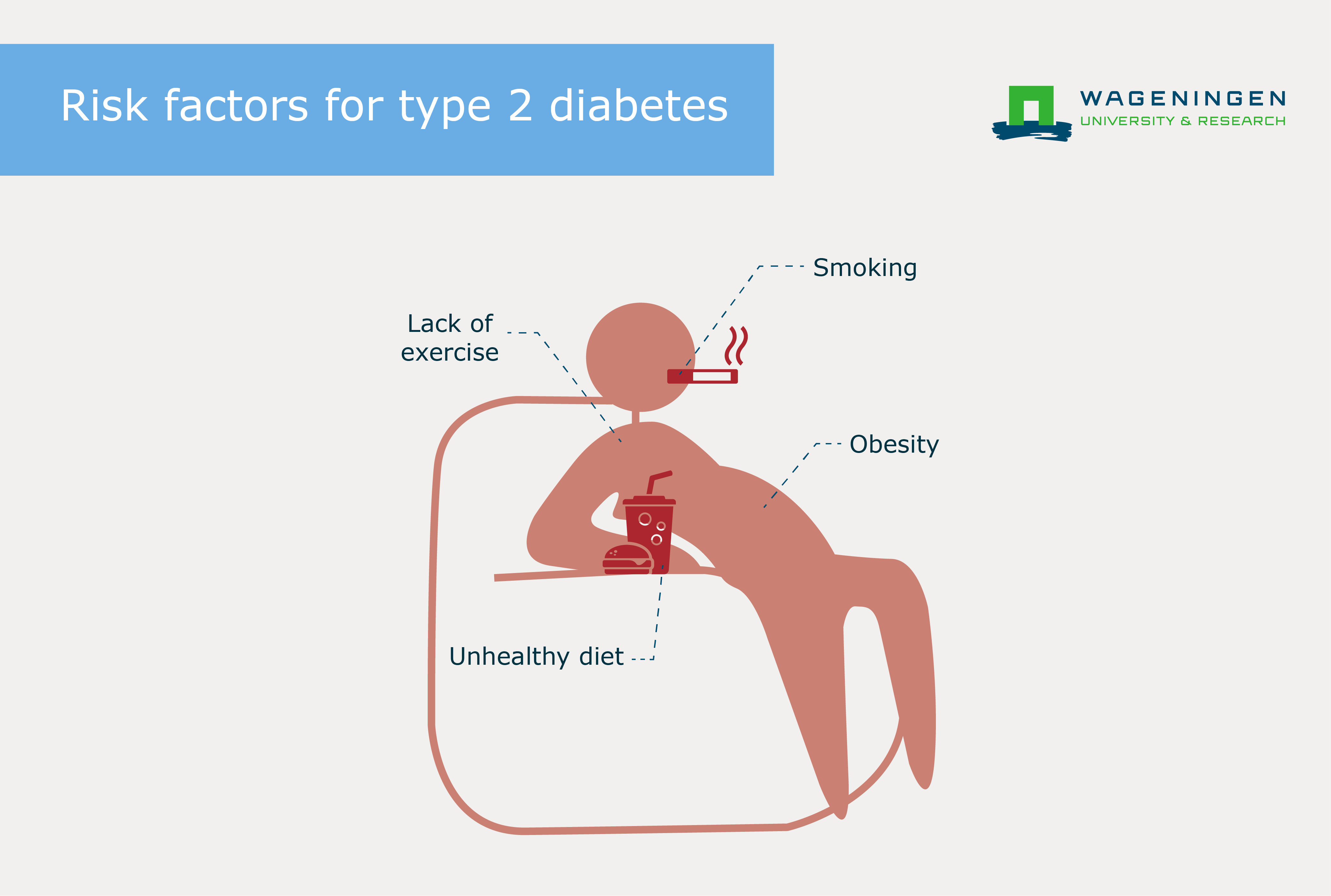
To reduce the number of people developing type 2 diabetes, Wageningen University & Research will make use of the Global One Health approach. We already know that we need to promote healthy diet and exercise as part of daily life and leisure time. However, behaviour is difficult to adjust in practice. This requires a joint effort by behavioural psychologists, medical specialists, nutritionists and policy officers.

By working on Global One Health, Wageningen University & Research is addressing these health risks while illustrating the interrelationships and interdependence between health, nutrition, society and environment. By using a chain approach we make an essential contribution to improving the health of people, animals and plants.
